States where the most people live in maternal health care deserts
Published 6:00 am Friday, October 29, 2021
Africa Studio // Shutterstock
States where the most people live in maternal health care deserts
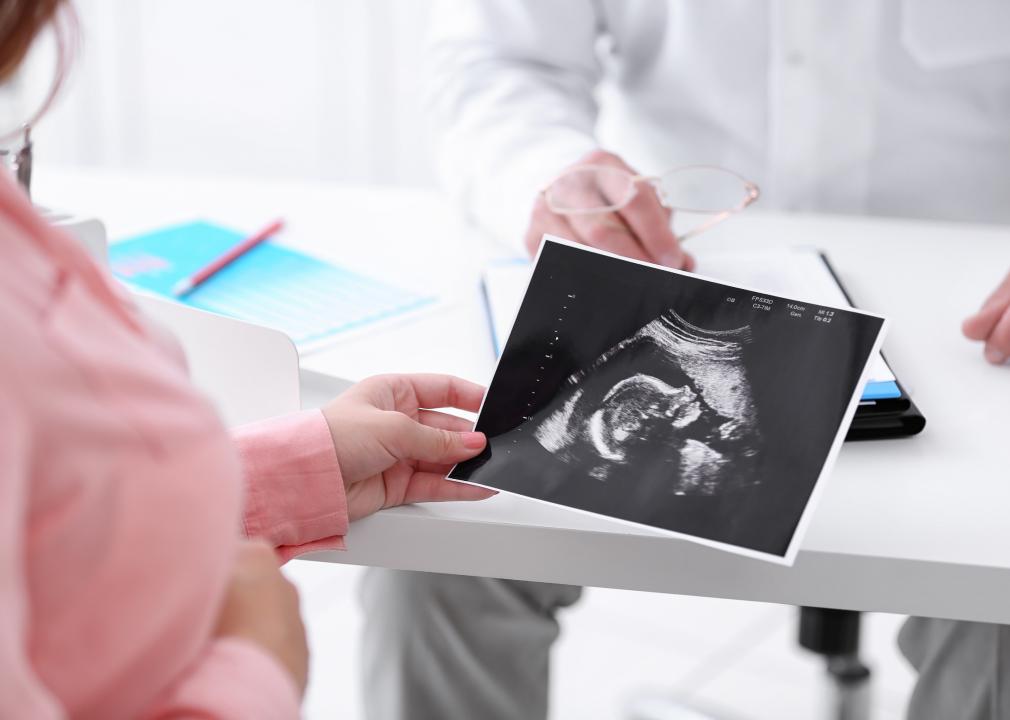
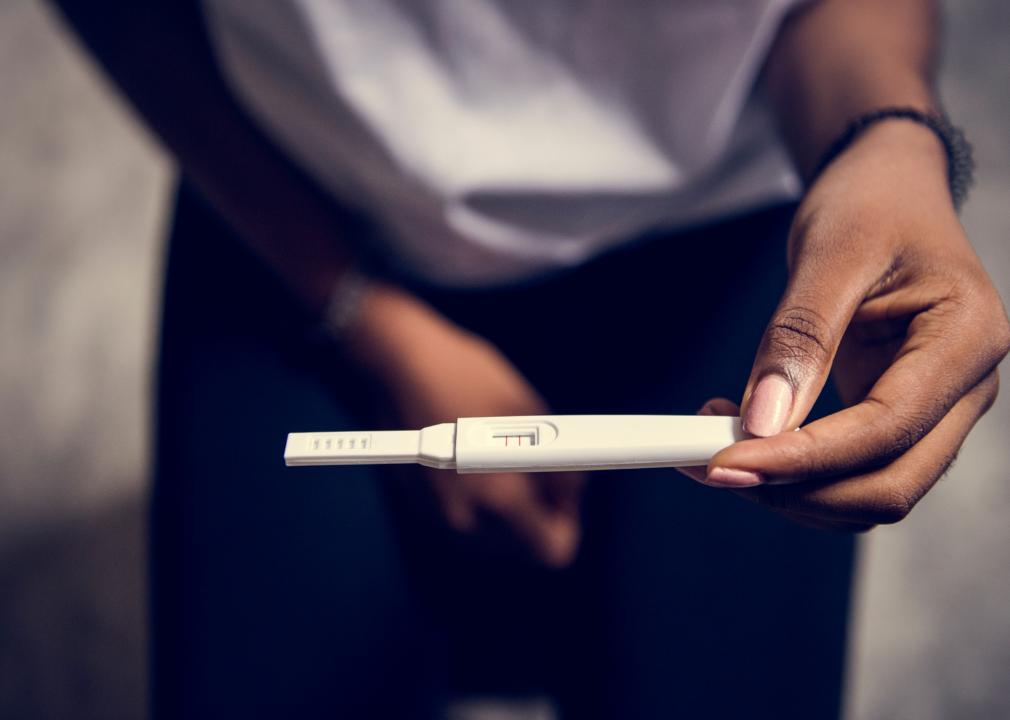
Compared to other developed nations, the United States regularly ranks among the worst countries for maternal and infant health outcomes. Childbirth outcomes are often tied to a birthing parent’s circumstances, fueling wide disparities at the geographic, demographic, and income levels.
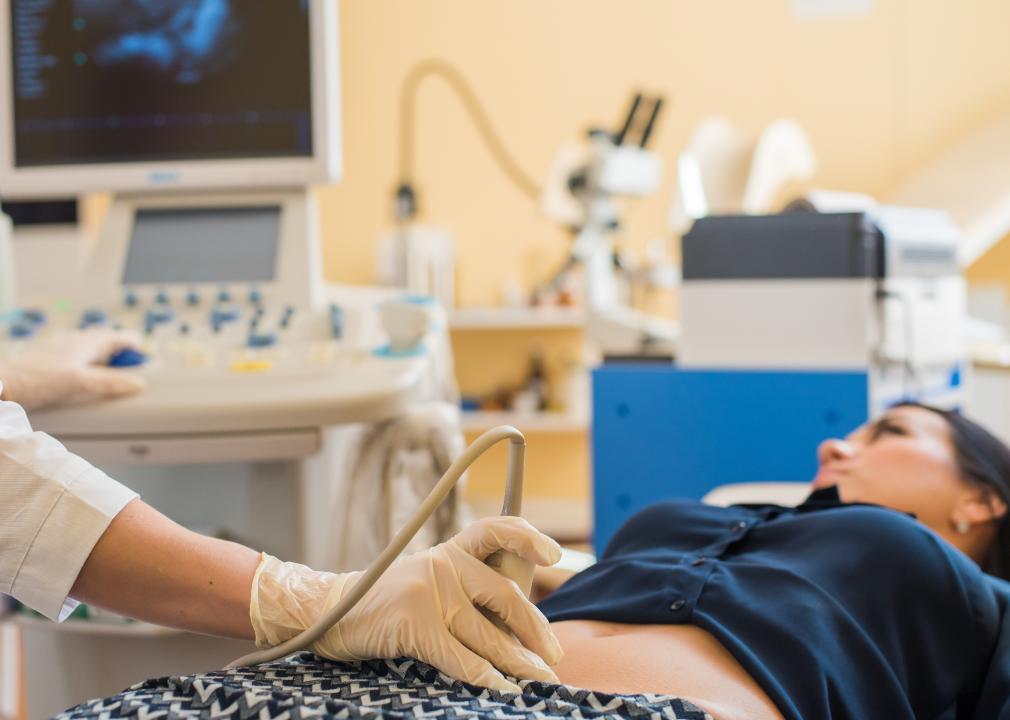
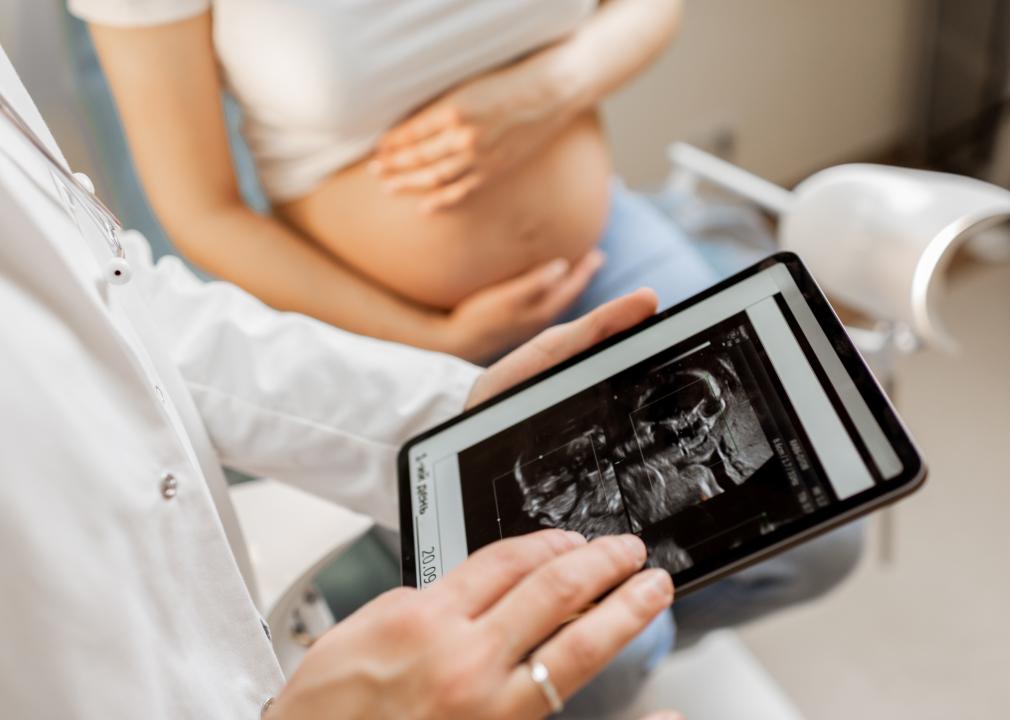
Research has shown that access to prenatal care, family planning services, and other contraceptive resources decreases maternal and infant mortality. However, an increasing number of counties throughout the country are losing access to obstetric care. Aging populations, limited staff, and low reimbursement rates for Medicaid patients are factors that have made rural hospital birth units costly to operate.
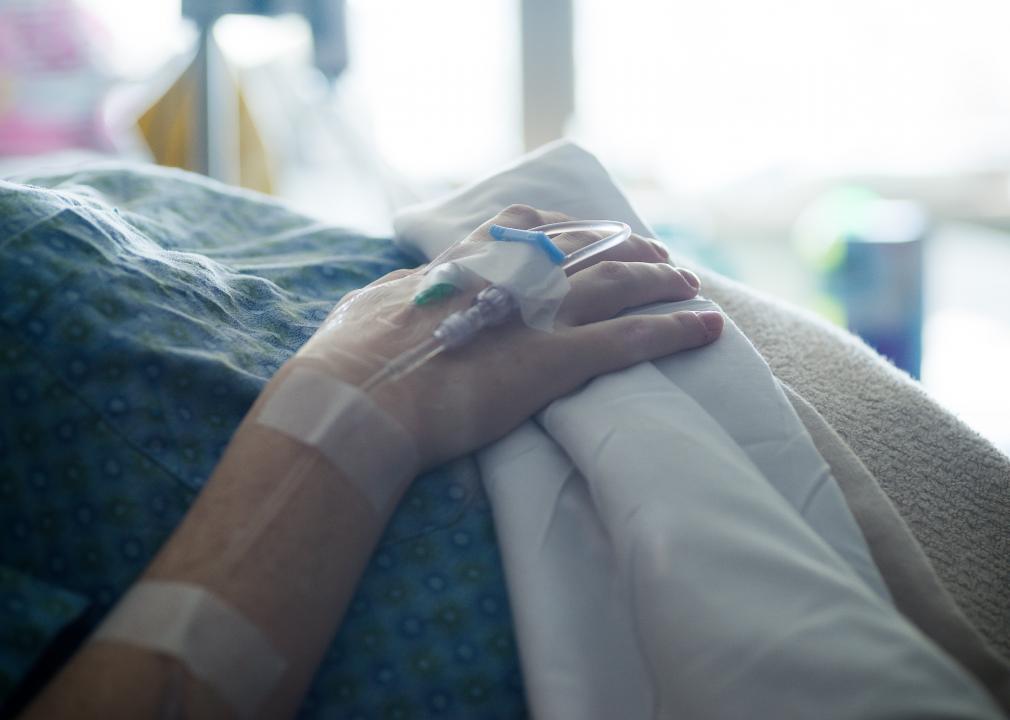
Even in areas with access to maternal care, other challenges like poverty, limited transit, lack of insurance, and systematic racism can put families at risk of poor maternal and infant health outcomes. Estimates from the CDC show that 60% of pregnancy-related deaths in the U.S. are preventable, but inadequate treatment and identification of health risks contribute to hundreds of maternal deaths annually.
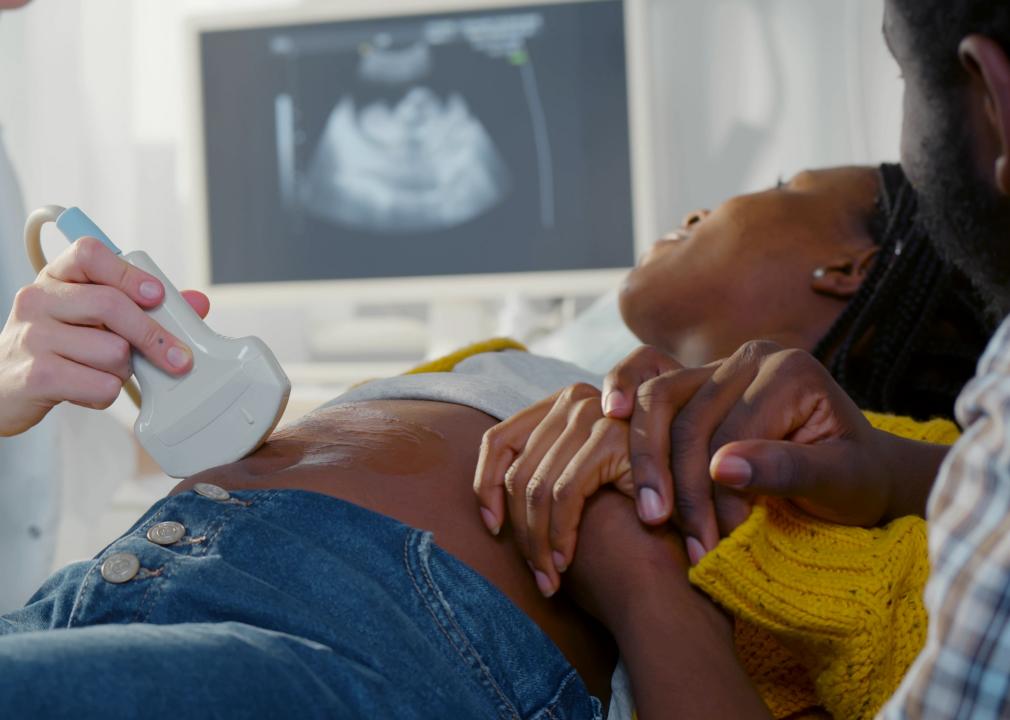
Pregnant Black people face disproportionate risks when giving birth. The infant mortality rate for Black children in the U.S. is double the rate for white children. Maternal mortality rates show similarly grim patterns, with 44 deaths per 100,000 live births among Black people compared to 17.9 per 100,000 live births for white people.
Stacker followed the March of Dimes’ definition of a maternity care desert, including counties with no hospitals with obstetric care, OB/GYNs, or certified nurse-midwives. To identify affected counties, Stacker analyzed the Area Health Resource Files from the Health Resources and Services Administration and merged this data with county-level birth data collected by the National Vital Statistics System to calculate how many births in each state are to parents who live in maternal health care deserts.
Stacker also used 2020 Census population data to calculate what percentage of a state’s population lives in counties without access to maternal health care. Stacker used population data across all sexes and ages to include county-level demographic data and more deeply compare racial disparities—although maternal health care deserts have a disproportionate impact on people between the ages 15–44, who can become pregnant.
Keep reading to learn about the challenges facing maternal health care in 15 states and how state policies and community-driven programs seek to bridge rural and demographic health care disparities.
You may also like: Most prevalent chronic conditions in American seniors
![]()
Helen Sushitskaya // Shutterstock
#15. Idaho
– Percent of state’s births to parents who live in maternal health care deserts: 9.9% (2,142 births)
– Population who lives in maternal health care desert: 10.3%
— 10.3% of state’s white population
— 2.5% of state’s Black population
— 10.0% of state’s Native American population
— 12.5% of state’s Hispanic population
— 4.4% of state’s Native Hawaiian/Pacific Islander population
— 3.2% of state’s Asian population
With obstetric services limited in rural areas, research has shown that accredited, midwife-led birth centers offer patients with low-risk pregnancies meaningful options outside of a hospital setting. However, Idaho is one of 11 states that don’t regulate birth centers, meaning Medicaid and some commercial insurances won’t cover the costs of childbirth. Although birth centers are the setting for only a tiny portion of the state’s births, midwives in Idaho and other Western states are working to improve health care access for rural, low-risk patients.
Prostock-studio // Shutterstock
#14. Montana
– Percent of state’s births to parents who live in maternal health care deserts: 10.8% (1,227 births)
– Population who lives in maternal health care desert: 11.3%
— 11.3% of state’s white population
— 5.6% of state’s Black population
— 15.7% of state’s Native American population
— 6.8% of state’s Hispanic population
— 7.0% of state’s Native Hawaiian/Pacific Islander population
— 4.5% of state’s Asian population
About 44% of Montana’s population lives in rural areas. With counties as large as 5,500 square miles, even pregnant people lucky enough to live in counties with maternal health access can still find themselves navigating long distances for prenatal care. Montana is working toward bridging the gaps in maternal care access: Funding from HRSA and the state’s public health department established the Montana Obstetrics and Maternal Support Program, which provides obstetric training for rural GPs, supports mobile clinics, and scales up telemedicine offerings.
nimito // Shutterstock
#13. Louisiana
– Percent of state’s births to parents who live in maternal health care deserts: 11.2% (6,434 births)
– Population who lives in maternal health care desert: 11.7%
— 13.6% of state’s white population
— 9.5% of state’s Black population
— 14.6% of state’s Native American population
— 7.6% of state’s Hispanic population
— 8.7% of state’s Native Hawaiian/Pacific Islander population
— 3.5% of state’s Asian population
Louisiana was one of the first states to implement a nurse-family partnership program. In 90% of the state’s parishes, eligible people pregnant for the first time are paired with specially trained nurses until the child’s second birthday. Most participants are enrolled in Medicaid, and the median household income is $6,000 annually. 88% of babies in the program were born full-term, compared to the state’s average of 86.9% across all income levels.
Other efforts specifically target Black parents, who are four times more likely to die from pregnancy complications than white people in Louisiana. The first Black-owned birth center opened in Lafayette this year. The Maternal and Child Health Coalition in New Orleans has advocated for municipal/state health care policies and inclusive hospital hiring practices.
Juice Verve // Shutterstock
#12. Alaska
– Percent of state’s births to parents who live in maternal health care deserts: 12.4% (1,193 births)
– Population who lives in maternal health care desert: 12.2%
— 7.6% of state’s white population
— 5.0% of state’s Black population
— 34.6% of state’s Native American/Alaska Native population
— 9.0% of state’s Hispanic population
— 6.3% of state’s Native Hawaiian/Pacific Islander population
— 14.3% of state’s Asian population
Alaska has a lower maternal mortality rate than the rest of the country, at 8.3 per 100,000 live births. However, for the Alaska Native population, this figure jumps to 19.2 per 100,000 live births. The Indian Health Service is the primary provider of culturally conscious health care in Indigenous communities, but its limited funding means facilities don’t always provide obstetric care. Pregnant Indigenous people who travel to seek care from traditional hospitals may also find institutional racism ingrained in their treatment.
Beyond racial disparities, some communities in Alaska are not even within driving distance of a hospital with obstetric services. Facilities have sought to bridge these gaps, like a prematernal home in Bethel where pregnant people from interior regions can live for a month before their due date.
Petrovich Nataliya // Shutterstock
#11. Iowa
– Percent of state’s births to parents who live in maternal health care deserts: 14.7% (5,444 births)
– Population who lives in maternal health care desert: 15.6%
— 17.3% of state’s white population
— 2.6% of state’s Black population
— 7.8% of state’s Native American population
— 8.2% of state’s Hispanic population
— 9.0% of state’s Native Hawaiian/Pacific Islander population
— 3.4% of state’s Asian population
In 2019, Iowa was one of nine states to receive a grant from HRSA to address disparities in maternal health. The state has seen rising maternal death rates over the past two decades, and over 30 hospital birth units have closed in the state since 2000. The 2020 census revealed a declining birth rate across America, and in Iowa counties with aging populations, hospitals lose money in the operation of local birth centers. It’s an issue that’s even more prevalent in counties where a high proportion of births are funded through Medicaid since private insurance payments to hospitals are often greater than Medicaid rates.
You may also like: Worst states for health care
Rawpixel.com // Shutterstock
#10. Alabama
– Percent of state’s births to parents who live in maternal health care deserts: 15.3% (8,703 births)
– Population who lives in maternal health care desert: 16.2%
— 17.9% of state’s white population
— 13.2% of state’s Black population
— 19.1% of state’s Native American population
— 13.1% of state’s Hispanic population
— 8.9% of state’s Native Hawaiian/Pacific Islander population
— 5.7% of state’s Asian population
Alabama finally decriminalized midwifery in 2016, after the practice had been illegal for over four decades, although certified nurse-midwives were allowed to work in hospital settings. This decriminalization has promoted the resurgence of Alabama’s rich midwifery history. Under Jim Crow laws, Black parents couldn’t access white hospitals, and Black midwives played a crucial role in overseeing births. Today, in a state where Black people are nearly five times more likely to die during pregnancy than white people, reproductive justice advocates believe historic midwifery models of care could better serve pregnant Black patients, especially in rural areas.
Reshetnikov_art // Shutterstock
#9. Nebraska
– Percent of state’s births to parents who live in maternal health care deserts: 16.1% (4,034 births)
– Population who lives in maternal health care desert: 16.9%
— 18.7% of state’s white population
— 3.7% of state’s Black population
— 37.6% of state’s Native American population
— 11.9% of state’s Hispanic population
— 19.3% of state’s Native Hawaiian/Pacific Islander population
— 3.1% of state’s Asian population
Nebraska’s Maternal Infant Early Childhood Home Visiting program is a community health initiative aimed at pregnant individuals and families with children under 5. The program supports parents at risk of poverty, substance abuse, exposure to violence, or other challenges by pairing them with counselors who promote positive parenting techniques. At the national level, the Tribal Home Visiting program provides grants to Native American tribes to offer similar, culturally conscious services.
Dollydoll29 // Shutterstock
#8. Oklahoma
– Percent of state’s births to parents who live in maternal health care deserts: 16.7% (8,205 births)
– Population who lives in maternal health care desert: 18.0%
— 19.7% of state’s white population
— 7.9% of state’s Black population
— 27.3% of state’s Native American population
— 11.1% of state’s Hispanic population
— 4.4% of state’s Native Hawaiian/Pacific Islander population
— 3.4% of state’s Asian population
Since 2010, 14 hospital birth centers have closed in Oklahoma. In rural hospitals across the country, balancing the cost of keeping trained obstetric staff on call with the dwindling birth rates in rural areas has left large swaths of the state without hospitals with birth units. Oklahoma is also one of the worst states for maternal mortality, with 2018 data showing 30.1 maternal deaths per 100,000 live births, compared to 17.4 nationally. A recently formed maternal mortality review committee reviewed eight maternal death incidents in the state and found that seven of those cases were preventable with timelier interventions.
Dragana Gordic // Shutterstock
#7. Missouri
– Percent of state’s births to parents who live in maternal health care deserts: 17.9% (12,881 births)
– Population who lives in maternal health care desert: 17.9%
— 20.7% of state’s white population
— 3.9% of state’s Black population
— 22.0% of state’s Native American population
— 11.1% of state’s Hispanic population
— 22.2% of state’s Native Hawaiian/Pacific Islander population
— 3.7% of state’s Asian population
A report from Missouri’s Office of Rural Health revealed that pregnancy-related deaths were 47% higher in rural areas than urban areas. Nine of the 10 Missouri counties with the highest infant mortality rate are considered rural. As an increasing number of hospitals close, nonprofit health care systems like Missouri Highlands have sought to expand their presence in rural parts of the state. Missouri laws now allow nurse practitioners to work up to 75 miles away from a collaborating physician, expanding a clinic’s rural reach.
RossHelen // Shutterstock
#6. North Dakota
– Percent of state’s births to parents who live in maternal health care deserts: 19.7% (2,072 births)
– Population who lives in maternal health care desert: 21.1%
— 21.6% of state’s white population
— 3.8% of state’s Black population
— 36.0% of state’s Native American population
— 15.6% of state’s Hispanic population
— 7.4% of state’s Native Hawaiian/Pacific Islander population
— 6.7% of state’s Asian population
In North Dakota’s 2016 Health Assessment Report, the state outlined priority areas to address maternal and infant health, including reducing tobacco use among pregnant people, increasing the breastfeeding rate, and reducing disparities in infant mortality. Data from 2014–2018 showed that Native American infants in the state were twice as likely to die than white infants. Native American people in North Dakota were also less likely to receive maternal care in the first trimester than white people, and at least 6% of pregnant Native Americans received no prenatal care at all.
You may also like: Healthiest states for seniors
KieferPix // Shutterstock
#5. West Virginia
– Percent of state’s births to parents who live in maternal health care deserts: 19.7% (3,465 births)
– Population who lives in maternal health care desert: 21.1%
— 21.9% of state’s white population
— 13.2% of state’s Black population
— 18.6% of state’s Native American population
— 13.8% of state’s Hispanic population
— 11.8% of state’s Native Hawaiian/Pacific Islander population
— 5.3% of state’s Asian population
There is only one OB/GYN in central West Virginia specializing in high-risk pregnancies, and the doctor there openly advocates against abortion. For high-risk patients, abortion can be a legitimate consideration for preventing mortality, and the second-closest OB/GYNs with similar specialties are over an hour away, leaving limited options for pregnant people in need of specialized care.
West Virginia leaders recently announced a $1 million grant from the U.S. Department of Health and Human Services to support the state’s Rural Maternity and Obstetrics Management Strategies Program. The program collects data, builds health care networks, determines regional approaches to risk-aware care, and supports telehealth to provide comprehensive maternal care in rural communities.
LightField Studios // Shutterstock
#4. Arkansas
– Percent of state’s births to parents who live in maternal health care deserts: 22.1% (8,014 births)
– Population who lives in maternal health care desert: 23.4%
— 26.2% of state’s white population
— 17.1% of state’s Black population
— 22.3% of state’s Native American population
— 14.1% of state’s Hispanic population
— 9.6% of state’s Native Hawaiian/Pacific Islander population
— 8.7% of state’s Asian population
Arkansas’s health department provides 5,000 patients with prenatal care annually through local health clinics, which provide services including family planning, STD testing, and prenatal education and counseling. The state’s Antenatal and Neonatal Guidelines, Education and Learning System (ANGELS) program provides telemedicine training to physicians and other specialists on managing high-risk pregnancies. Before the program’s establishment, high-risk patients were referred to specialists concentrated in urban centers. The program has minimized long commutes for prenatal care and equipped rural physicians with the tools they need to oversee riskier pregnancies.
Debra Anderson // Shutterstock
#3. Kentucky
– Percent of state’s births to parents who live in maternal health care deserts: 22.4% (11,821 births)
– Population who lives in maternal health care desert: 23.8%
— 26.7% of state’s white population
— 6.4% of state’s Black population
— 20.7% of state’s Native American population
— 12.3% of state’s Hispanic population
— 10.8% of state’s Native Hawaiian/Pacific Islander population
— 4.3% of state’s Asian population
Mary Breckinridge founded Frontier Nursing Service almost a century ago, training nurses on horseback to provide vital midwifery care to isolated communities in Kentucky’s Appalachian Mountains. Breckinridge founded Hyden Hospital and Health Center, and in 2020, the hospital moved from the eastern part of the state to Versailles, outside Lexington. The move coincided with a decline in the number of rural hospitals in Appalachia, exposing the region’s limited maternal care infrastructure for maternal care.
Kentucky is lifting its previously stringent regulations on midwifery: Before 2019, the last Certified Professional Midwife permit was issued in 1975, but midwives can now get permits and reach families who may not otherwise receive prenatal care. Kentucky also lifted a collaborative agreement rule for certified nurse-midwives, meaning they no longer have to work with a regional physician to practice in an area.
Tyler Olson // Shutterstock
#2. South Dakota
– Percent of state’s births to parents who live in maternal health care deserts: 23.2% (2,715 births)
– Population who lives in maternal health care desert: 22.6%
— 21.8% of state’s white population
— 4.8% of state’s Black population
— 41.2% of state’s Native American population
— 15.7% of state’s Hispanic population
— 25.2% of state’s Native Hawaiian/Pacific Islander population
— 5.8% of state’s Asian population
In 2016, the Rosebud Sioux Tribe sued the federal government for closing the emergency department of the reservation’s only hospital. Services like obstetric care were disrupted, and patients were diverted to alternative facilities ranging from 45–220 miles away. A federal appeals court recently ruled in the tribe’s favor, but the legal battle highlighted the challenges facing underfunded Indian Health Service hospitals.
Across South Dakota, pregnant Native Americans face poorer outcomes than pregnant white people. The maternal mortality rate for Indigenous people is 121 per 100,000, compared to 44 per 100,000 among white parents in the state. Access to transportation, eligibility for Medicaid, and systematic racism are some of the core factors causing this disparity. Proposed solutions to these complex challenges include reservation-based birthing centers, supporting traditional birth methods, and deploying telemedicine.
Rachaphak // Shutterstock
#1. Mississippi
– Percent of state’s births to parents who live in maternal health care deserts: 23.6% (8,484 births)
– Population who lives in maternal health care desert: 23.5%
— 23.8% of state’s white population
— 23.9% of state’s Black population
— 51.3% of state’s Native American population
— 19.1% of state’s Hispanic population
— 11.9% of state’s Native Hawaiian/Pacific Islander population
— 5.6% of state’s Asian population
According to the CDC, Mississippi has the country’s highest infant mortality rate, at 9.7 deaths per 1,000 live births. A report from the state’s department of health shows that the high mortality rate connects to a large number of preterm births. Effective ways to reduce preterm births include screening pregnant people for conditions that may put them at a higher risk.
Community-driven health measures have been shown to improve infant health outcomes, and Mississippi has begun pilot programs to coordinate prenatal support for pregnant people living in poverty. However, Mississippi is also at the center of a major Supreme Court battle over whether it is constitutional to ban abortion after 15 weeks.
You may also like: America’s most common ticks and how to identify them